Opioids and Naloxone
From 2020 to 2021, opioid-related deaths in Canada nearly doubled increasing from 3,747 to 7,362. In 2021, Hamilton’s opioid-related death rate was 47% higher than the Ontario provincial rate. It is more important now than ever to familiarize yourself with the steps you can take to help keep those experiencing opioid-overdose alive until emergency services arrive.
What are Opioids?
Opioids are a class of drugs naturally found in the opium poppy plant. They work in the brain to produce a variety of effects, including pain relief, relaxation, or feelings of being happy, or “high”. Opioids are highly addictive, and they can be found in both prescribed and illicit forms. They are most often prescribed to treat pain, but they are also widely misused. Opioids are commonly found as tablets, capsules, skin patches, powder, and as a liquid (used orally or by injection).
Opioids trigger the release of endorphins, your brain’s “feel good” chemical. When you take opioids, your body lowers the regular production of endorphins causing users to seek higher doses of opioids to get the same effect. This is what causes addiction.
Opioid Names
The most commonly used opioids are:
- Prescription opioids, such as OxyContin and Vicodin
- Fentanyl, a synthetic opioid 50 times stronger than heroin and 100 times stronger than Morphine
- Codeine
- Morphine
- Oxycodone
- Hydromorphone
Opioids Risk
Even when prescribed to treat specific conditions or pain, there are serious side effects and risks of using opioids:
- Opioid dependence
- Regular use of prescribed medication can increase tolerance requiring higher doses to elicit the same effects.
- Increasing doses beyond an individual’s limits can lead to overdose.
- Overdose
- Overdose occurs when you take too much of an opioid.
- Opioids affect the part of the brain that controls breathing. When you take more than you can handle, your breathing slows to dangerously low rates leading to unconsciousness and even death.
- Illicitly purchased opioids are often not pure and can be mixed with other more potent and addictive drugs such as fentanyl.
- When individuals do not know the strength of the drugs they are using, overdoses are more likely.
- Two milligrams of pure fentanyl – the amount of about four grains of salt – is enough to kill an adult. Carfentanil, an opioid used by veterinarians, is 100 times more toxic than fentanyl.
- Life-threatening withdrawal symptoms in babies born to mothers taking opioids
Opioid Overdoses
From January 1 to June 19, 2022, Hamilton Paramedic Services responded to 327 incidents related to suspected opioid overdoses. Over the course of the COVID-19 Pandemic, the number of suspected opioid overdoses increased from 565 incidents in 2020 to 914 incidents in 2021. This increase in opioid overdoses has been seen in communities across Canada. Several factors may have contributed to a worsening of the opioid crisis during the COVID-19 pandemic, including increasingly potent drug supplies, increased feelings of isolation, stress and anxiety, and decreased access to services for people who use drugs.
Signs and symptoms of opioid overdose
- Difficulty walking, talking, staying awake
- Blue lips or nails
- Very small pupils
- Cold and clammy skin
- Dizziness and confusion
- Extreme drowsiness
- Choking, gurgling or snoring sounds
- Slow, weak or no breathing
- Inability to wake up, even when shaken or shouted at
What to do if you think someone is overdosing
- Try to wake the person up. Shout and shake them to keep them awake. If no response, grind your knuckles on their breast bone for 5-30 seconds.
- Call 911 immediately.
- Administer naloxone if available. Inject the full dose, or if it is a spray, give half up each nostril. Naloxone should be administered even if you do not know what drug the person has taken. However, naloxone is only effective against opioid overdoses. Giving naloxone to a person that is unconscious because of a non-opioid overdose is unlikely to cause harm.
- Try to keep the person awake and breathing.
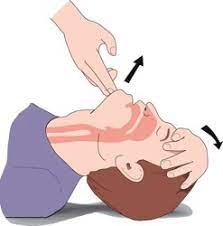
- Check for breathing. If they have stopped breathing, provide rescue breaths: tilt the head back, open mouth, pinch the nose. Continue to provide 1 breath every 5 seconds until help arrives. If they have lost their pulse (heart is not pumping) give 30 chest compressions and two rescue breaths (if you are trained and comfortable doing so). Continue doing so until help arrives.
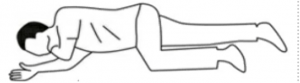
- If breathing and pulse return, lay the person on their side in the Recovery Position to prevent choking: top leg and bottom arm bent to prevent rolling, and top arm bent and under the chin to support the head.
- Stay with the person until emergency assistance arrives.
- If there is no response 2-3 minutes after the first dose, administer another dose of naloxone.
Good Samaritan Drug Overdose Act
The Good Samaritan Drug Overdose Act became law on May 4, 2017. The Act can protect you from:
- Charges for possession of a controlled substance (i.e. drugs)
- Breach of conditions regarding simple possession of controlled substances in
- pre-trial release
- probation orders
- conditional sentences
- parole
It applies to anyone seeking emergency support during an overdose whether they stay or leave from an overdose scene before emergency services arrive.
The act does not provide legal protection against more serious offences:
- outstanding warrants
- production and trafficking of controlled substances
- all other crimes not outlined in the Act
What is Naloxone and How to administer it?
Naloxone is a medication that quickly reverses an overdose by blocking the effects of opioids. It can restore breathing within 2 to 3 minutes in a person whose breathing has slowed or stopped from an opioid overdose.
Naloxone works. In 2019, 2000 people were revived with naloxone in the Hamilton community. The Mac Opioid Crisis Collective hosts Naloxone kit training workshops. Follow their Instagram and check out their website for training details.
Naloxone can be found in two main forms
- Nasal Spray
-
- Spray medication into the nose
- Auto-injector
-
- Inject medication into the outer thigh
- Check out this video by the American Medical Association on how to use Naloxone
Where to find Naloxone?
McMaster Special Constables and Emergency First Response Team (EFRT) carry naloxone nasal spray.
Naloxone kits are available without a prescription at local pharmacies, including King Medical Pharmacy, McMaster Health Campus Pharmacy, McMaster University Centre Pharmasave (in MUSC), Metro Pharmacy, all Shoppers Drug Marts, and Whitney Plaza Pharmacy.
Use this Government of Ontario Map to find out which pharmacies offer free naloxone kits and training on how to use them: https://www.ontario.ca/page/where-get-free-naloxone-kit
Community Resources For Opioid-use Cessation
- Alternatives for Youth: Substance-use services for youth aged 12-23 and their families
- 38 James Street South, 2nd Floor, Hamilton, Ontario L8P 4W6
- Phone: 905-527-4469
- E-mail: admin@ay.on.ca
- John Street Clinic: Specializes in methadone treatment for addictions to heroin or opiates such as morphine, Percocet, or Dilaudid. Medical consultation, assessment and referrals are available.
- 14 John St N, Hamilton, ON L8R 1G9
Phone: 905-522-7206
Accessibility: Fully Accessible
- 14 John St N, Hamilton, ON L8R 1G9
- Ontario Addiction Treatment Centre: Encourages long-term sobriety from all illicit substances
- 397 Main St E, Hamilton, ON
Phone:905-528-9889
- 397 Main St E, Hamilton, ON
- Sober Grid: combines peer support coaching, an online community, digital therapeutics and library of mental health resources for long term recovery
- Online App
- Canadian Centre on Substance Use and Addiction: non-governmental organization to provide national leadership on substance use and to advance solutions to address alcohol- and other drug-related harm
- Centre for Addiction and Mental Health (CAMH): CAMH provides a wide range of clinical care services for patients of all ages and families, with Access CAMH as your centralized point of contact.
Reference:
https://www.hamilton.ca/public-health/reporting/hamilton-opioid-information-system
https://www.cdc.gov/stopoverdose/fentanyl/index.html
https://www.canada.ca/en/health-canada/services/opioids/overdose.html
https://www.hopkinsmedicine.org/opioids/what-are-opioids.html
https://wellness.mcmaster.ca/your-health/alcohol-cannabis-tobacco-and-opioids/
https://www.hamiltonhealthsciences.ca/share/how-to-use-a-naloxone-kit/
https://www.camh.ca/en/health-info/mental-illness-and-addiction-index/naloxone
https://www.hamilton.ca/public-health/reporting/hamilton-opioid-information-system-deaths
Addictions, Alcohol, Cannabis, & Substances